(Reuters) – An influential panel of U.S. experts issued final recommendations on Monday reaffirming their controversial position that mammogram screening should start at age 50, but also said some women may benefit from screening starting at age 40. Under the U.S. Preventive Services Task Force guidelines, mammogram screening every two years for women 50 to […]
U.S. Preventive Services Task Force (USPSTF)
New mammography guidelines stick with screening from age 50
American Cancer Society CMO: Money-driven hospitals push for dangerous tests

Routine screening has been touted as the most effective way to stem cancer deaths, but it may instead put patients in harm’s way, according to American Cancer Society chief medical officer Dr. Otis Brawley. Speaking at a seminar last week, Brawley warned that hospitals recommending regular screening may be looking out for their profits rather than their patients.
Routine lung cancer screening gets federal panel’s OK for the 1st time
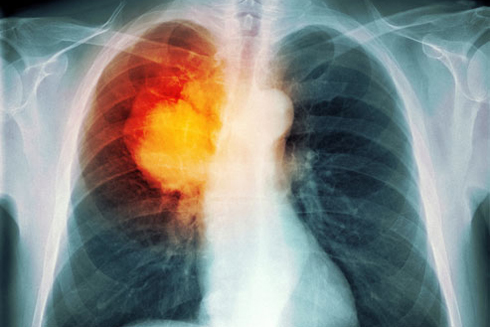
The U.S. Preventive Services Task Force made waves this week when it recommended for the 1st time that certain patients undergo annual low-dose CT scanning for lung cancer, paving the way for insurance companies to cover the tests.
Mixed messages on the merits of mammograms
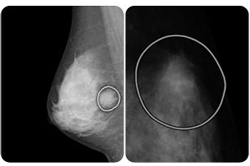
The latest published research on mammogram use and breast cancer trends in the U.S. offered mixed messages for women who must navigate betwen the dangers of missing mammograms as well as for getting over-treated as a result of them.
A new study released by the Radiological Society of North America warned that new federal recommendations regarding breast cancer screening could result in skipped mammograms and missed cancers.
Report: EKGs no help in preventing heart disease in low-risk patients, U.S. task force finds
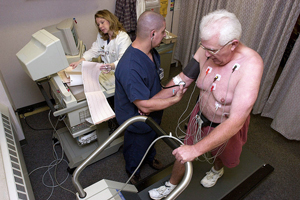
Physicians should reconsider using electrocardiography routinely in healthy patients without symptoms of heart problems, according to the latest recommendation from the U.S. Preventative Services Task Force.
The "incremental information" garnered from an EKG, whether testing at rest or during exercise, isn’t likely to produce data that would help a physician better understand a patient’s risk of coronary heart disease, according to the panel.
AMA rejects federal mammography guidance
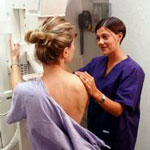
The American Medical Assn.’s House of Delegates updated its mammogram screening recommendation to include all women starting at age 40, flying in the face of guidance from the U.S. Preventative Services Task Force that caused a commotion among healthcare providers.
The USPSTF, an independent body funded and staffed by the U.S. Dept. of Health & Human Services, holds that routine mammogram breast cancer screenings are not necessary for women under the age of 50 who aren’t at increased risk.
Docs resist prostate test recommendation | MassDevice.com On Call

MASSDEVICE ON CALL — Primary care docs surveyed by Johns Hopkins University researchers say they’re unlikely to curtail their use of a test to detect prostate cancer, despite recommendations from the U.S. Preventive Services Task Force.
The USPSTF stirred up a controversy last year when it suggested that routine prostate-specific antigen tests for healthy men might do more harm than good.
USPSTF – It’s about time

The numbers are stark. According to the United States Preventive Services Task Force, for every man whose death from prostate cancer is prevented through PSA screening, 40 become impotent or suffer incontinence problems, two have heart attacks and one a blood clot.
Then there’s the psychological harm of a “false positive” test result, which is 80 percent of all “positive” tests. They lead to unnecessary worry, follow-up biopsies, physical discomfort and even harm. Final grade: D.
Prostate cancer: PSA test skipping advice creates outrage | MassDevice.com On Call

MASSDEVICE ON CALL — A nationwide urologists lobbying group largely discredited guidance from a U.S. Preventative Services Task Force recommending that physicians set aside a commonly used prostate cancer screening tool.
Known as the prostate-specific antigen test, or PSA, the tool may pose more risks than benefits, according to the panel.
Studies suggest new breast screening standards | MassDevice.com On Call

MASSDEVICE ON CALL — Two studies published today in the Annals of Internal Medicine could influence the standard of care for breast screening, which was called into question by a U.S. Preventive Services Task Force report in 2009.
That report suggested that annual mammograms might cause more harm than good because of increased false positives leading to unnecessary biopsies and further testing – not to mention considerable anxiety for patients.


