A "slapdash" system of reporting complications may be hiding the true dangers of robot-assisted surgery, according to a Johns Hopkins report published online this week in the Journal for Healthcare Quality.
Surgeons have performed around 1 million robot-assisted surgeries since 2000, but the FDA’s data notes only 245 total complications, including 71 deaths associated with the technology. That figure is far too low for the complex surgeries that typically include robotic technology, and the confusing nature of reporting standards may be obscuring some of the data, researchers said.
"The number reported is very low for any complex technology used over a million times," Johns Hopkins associate professor Dr. Martin Makary said in prepared remarks. "Doctors and patients can’t properly evaluate safety when we have a haphazard system of collecting data that is not independent and not transparent. There may be some complications specific to the use of this device, but we can only learn about them if we accurately track outcomes."
Furthermore, the researchers found a number of cases in which adverse events associated with the high-tech systems weren’t reported to the FDA until after they’d already made national headlines, sometimes long after the incidents had actually occurred. It’s likely that there are other incidents that remain unreported, the Johns Hopkins team said.
Determining the true dangers of robot-assisted surgery is increasingly important, especially given the soaring popularity of the technology. Between 2007 and 2011 robotic procedures in the U.S. increased more than 400% and internationally they rose more than 300%, according to the study. As of 2011 there were around 1,400 surgical robots in hospitals, nearly double the figure from just 4 years earlier.
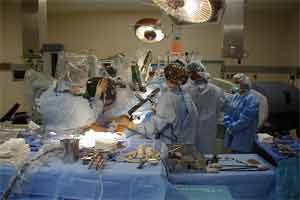
Minimally invasive robot-assisted surgery has been used to perform a variety of surgeries, including hysterectomies, gallbladder removals and mitral heart valve repairs, via remote-controlled instruments inserted into the body through small incisions. The surgeon directs the robot’s movements from a console, which is sometimes in another room.
Robotic devices can access smaller spaces than human hands and fingers can, the Johns Hopkins team noted, but some surgeons have complained that the technology reduces tactile sensation, making it harder to ‘feel out’ a procedure. A previous, anonymously conducted survey of surgeons found that 57% claimed they experienced an "irrecoverable operative malfunction" during a robot-assisted procedure, which forced them to resort to laparoscopy.
Standardized adverse event reporting needed
A lack of standardization and clarity in adverse event reporting may be keeping those complications hidden, the Johns Hopkins team warned.
For example, the study highlighted a rare complication in which surgeons mistakenly sliced a patient’s aorta because they couldn’t feel its firmness. It’s unclear, however, whether such an error should be filed as user error or a device flaw, and the FDA doesn’t track complications filed under surgeon error.
The study argued that those types of issues, although preventable with proper technique, should be tracked as device-related because they are more common with robotic surgery compared to conventional surgery. That way, they can also contribute to adverse-event tracking for robot-assisted procedures.
A false sense of security
The lack of proper tracking not only potentially dupes doctors, it may also give patients a false sense of the safety of robot-assisted surgery.
"We need to be able to give patients answers to their questions about safety and how much risk is associated with the robot. We have all suspected the answer has not been zero," Makary said. "We still don’t really know what the true answer is."
Recent studies have suggested the patients undergoing robotic surgery fare just as well as those who undergo laparoscopic procedures, although the robots hike the price of treatment.
"We need innovation in medicine and, in this country, we are tremendously good at introducing new technologies," Dr. Makary said. "But we have to evaluate new technology properly so we don’t over-adopt, or under-adopt, important advances that could benefit patients."
Gynecologic surgery leads robotic surgery death count
Johns Hopkins researchers examined the FDA’s databases, cross-referencing adverse events reports with court records and news reports. They found 8 adverse events that "were not appropriately reported to the FDA," they said. Five of those cases were never filed, they said, and 2 were filed only after the news media had caught on.
They further concluded that, of reported complications, gynecological procedures had the highest mortality rate, representing 22 of 71 deaths reported. Hysterectomies had the highest reported complications, representing 43% of injuries, most often excessive bleeding.
Robot makers in the court room
The study is not the 1st to raise concerns about the safety and efficacy of robot-assisted surgical systems. Device makers like Intuitive Surgical (NSDQ:ISRG) have recently found themselves in the spotlight and in the court room, facing questions about the dangers of the technology.
Earlier this summer Intuitive revealed an FDA warning letter in which the federal watchdog agency cited some "objectionable observations" about the company’s complaint handling and recall procedures.
In recent months the company, once a Wall Street darling, has also faced an FDA probe into surgical complication rates, an American Congress of Obstetricians & Gynecologists statement questioning the benefits of da Vinci surgery, a high-profile patient injury lawsuit painting the company as an aggressor, a surgical instrument crack warning and a shareholder class action lawsuit against the company and its leadership.

