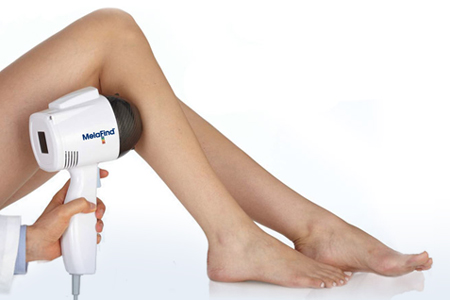
New York-based Mela Sciences (NSDQ:MELA) is hoping to secure insurance reimbursement for its MelaFind melanoma identification system, starting with coverage codes from the Centers for Medicare and Medicaid Services.
The Medicare nod would be a huge boon for Mela, which has for years been fighting for its place on the market. The company’s MelaFind system won FDA clearance in November 2011, a process that took more than 2 years, 2 FDA panel reviews and a citizens’ petition. Medicare coverage may be in place as early as January 2016, Mela said.
The company announced today that it filed documents to obtain a Current Procedural Terminology (CPT) code for Medicare Part B reimbursement, an important stepping stone to landing additional coverage from private insurers. Mela’s request will get review from the American Medical Assn.’s Editorial Panel, which will then get a pricing recommendation from the AMA’s Relative Value Scale Update Committee. CMS makes the final decision regarding approval and coverage levels.
"Our CPT application is the 1st concrete step in achieving our goal of obtaining insurance reimbursement for physician use of the MelaFind system," president & CEO Rose Crane said in prepared remarks. "MelaFind’s ability to improve diagnostic accuracy without increasing the number of biopsies, as demonstrated with the data presented at the 2014 American Dermoscopy Association Meeting is very meaningful to both patients and physicians and ultimately can save costs in the healthcare system. We believe our application makes a compelling argument in favor of receiving the CPT code and for obtaining reimbursement from CMS."
Mela’s handheld, non-invasive melanoma detection and identification system has been its primary revenue stream since the company discontinued its dental diagnostics operations in 2005. The device won CE Mark approval in the European Union in September 2011, paving the way for Mela’s return to the market.

