Kurt Dasse, the CEO of Waltham, Mass.-based Levitronix, counts a stint as chief scientific office for Thermo Electron Corp., better known today as Thermo Fisher Scientific as key to his professional career. His tenure at Thermo proved fateful, as it was there that Dasse came under the wing of the legendary George Hatsopoulos and his fervent devotion to starting new companies.
After Hatsopoulos retired, he helped Dasse found Levitronix, based on the magnetic levitation technology they’d worked on at Thermo. Levitronix, which makes the pumps used by Thoratec Corp. for its HeartMate series of implantable cardiac devices, also found applications for its bearingless motors in the semiconductor industry. In fact, just about any industry that deals with precious fluids — and what’s more precious than blood? — could probably find a use for the seemingly magical little devices.
MassDevice caught up with Dasse the day President Barack Obama signed the final piece of the healthcare reform act into law. He filled us in on the origins of his company, why its technology is so useful in medical devices and other fields, and gave us his take on how healthcare reform might drive consolidation in the medical device industry.
MassDevice: Can you give us a primer on Levitronix’s corporate history?
Kurt Dasse: One of the co-founders of what now is called Levitronix is George Hatsopoulos. George Hatsopoulos was the founder, CEO and chairman of Thermo Electron Corp., which is now Thermo Fisher Scientific (NYSE:TMO). While at Thermo Electron, I had worked for a company called Thermo Cardiosystems, which was one of the 24 public companies under Thermo Electron Corp., with a focus on heart assist devices [Eds. note: Thermo Cardiosystems merged with Thoratec Corp. (NSDQ:THOR) in 2001.] I spent much of my career focused on that area and was promoted to chief scientist at Thermo Electron. At one point I said to George, “What do you love about running a big company like this?” He said, “I love creating new businesses.” And when I said, “What don’t you like?” he said, “Well, I’m 70 years old and it gets very wearing running a $4 billion company.” So I said, “Well, how would you like to create a new business?” So George did retire from Thermo Electron and we started a company that is actually called Pharos LLC. Pharos is actually a business that is a continuation of George’s desire to create new businesses. The first business we created within Pharos is Levitronix.

George Hatsopoulos
We started Levitronix in 2001 and it does relate back to my earlier experience with Thermo Cardiosystems, because when we were developing blood pumps for assisting the heart, we felt that there were three potential failure points, which include valves, flexing diaphragms and bearings. Your heart is beating about 40 million times a year, and therefore this blood pump would have to either flex or cycle these components 40 million times a year without having any access to lubrication or being able to salvage those components. At some point they’re going to fail, so our goal was to design a pump that would have none of these failure components; no valves, no diaphragms, no bearings, no shafts, no seals, nothing that would wear out. That’s precisely the technology that we ultimately developed, a bearingless motor where the rotating component of the pump is magnetically levitated. We use electro-magnetic forces to cause it to be levitated, but at the same time we can center the spinning component and then cause it to rotate, thereby imparting the torque to pump blood or any other precious fluid.
So you take the pump and you simply drop it into a receptacle. The pump is comprised of a top and lower housing and only one more piece, which is that rotating spinning component inside the pump chamber. Within that spinning component is a magnet; when we create electro-magnetic forces it causes that spinning component to be raised or levitated and then to rotate such that it’s freely suspended and rotating within the magnetic fields. It is the impeller and also the rotor of the motor. It’s really exciting, because it is a platform technology that has many medical applications but, in the same breath, has many industrial applications.
We started in the semiconductor field in wet-bench processing. The best way of describing it is to think of an old-fashioned jukebox. You’ve got the robotic that picks up the 45 and drops it onto a turntable, which actually in the semiconductor field is called a chuck. The 45 is actually a wafer that’s been dropped on it before it’s been cut up into chips. So now that wafer is rotating on that chuck and they need precious fluids to be recirculated that do not have any contaminants, particles, bearing particulates or lubricants such that they can process that wafer. The wafer will be at different levels, with one solution one level which might be an alkali; you have another solution that might be an acid at another level and eventually a wash. It’s a process that has to be done in an absolutely clean environment and they like to recirculate the solutions, so you need a pump that will do this in a highly reliable and clean fashion.
This has gone from wet-bench processing to photo-lithography applications to an application called chemical-mechanical planarization. In this case, an easy analogy is to think of waxing your car in the old days. You would use a buffer and a polish, and so in this case you have a wafer where we as a pump deliver a slurry, which is a polish to the wafer, and then what we’re doing is planing, in nanoscale, imperfections in the wafer such that it’s polished perfectly smooth. The slurry solutions are very much like blood. Blood has platelets in it and if triggered the platelets will agglomerate and they’ll clump. Slurries also have nanoparticles that have the affinity to try to aggregate and if they do they will scratch the wafer and significantly reduce the yield of the chips.
MassDevice: How large a portion of Levitronix’s business is the medical device segment?
KD: It’s roughly 50 percent and growing rapidly now.
MassDevice: Levitronix makes the pump used in Thoratec’s ventricular assist device. What about the pump makes it suitable for that application?
KD: There are actually multiple applications where we provide pumps to Thoratec. They currently have a device called HeartMate II, which is an axial flow pump that’s pretty much dominating the market today. We are working on the next generation, HeartMate III, that would be another implantable pump where the value of the pump is that it’s highly reliable and the life of the pump might be significantly longer than devices that are currently available.
 Photo by Connor Gleason
Photo by Connor Gleason
We also provide our CentriMag blood pump to Thoratec. HeartMate II and HeartMate III are designed for long-term implantable patients with chronic congestive heart failure disorders. There are other patients that suffer from heart attacks or from other forms of cardiogenic shock in which the onset is very quick. They’re acute conditions that are potentially reversible if they can be supported for weeks to a month. And so CentriMag is a device that is used as a bridge to decision, where the decision is, once you’ve stabilized the patient, they either recover, go on to transplant or to a long-term system. It’s a device that provides the hemodynamic support to keep these patients stable until they can make a decision as to the outcome.
We currently are marketing a pediatric version of that device, for patients that need support for up to 30 days that’s an external system. We have what we call cannula, tubing, that is attached to the heart, generally in an open-heart surgical setting, and we plumb into the system and support the patient in the intensive care setting (or, in some cases in Europe, outside the intensive care setting) for periods of generally up to a month, until they either recover or go on to another therapy.
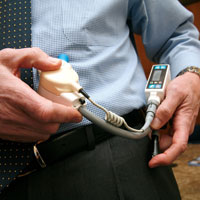 Photo by Connor Gleason
Photo by Connor GleasonWe are working on some really exciting things that have never been done before. The next series of products we’re working on; by the way, most of this has been funded by the National Institutes of Health, virtually everything I’m telling you about, they’re actually funding our pediatric trials. The next series of products are really exciting in that we’ve taken the pump we just talked about and we’ve integrated that with hollow-fiber technology that can be used for a lung; it’s a pump-lung. We have the first family of devices which would be used for short-term support of patients with potentially reversible respiratory problems, but we’re also working on a wearable pump-lung. That would be something that patients with emphysema or chronic lung disease could actually wear, where they have little ability to do gas exchange or ventilate. We would actually directly do that gas exchange to the blood. It would hopefully be like a light switch, where they’re struggling to breathe, unable to get sufficient oxygen into the blood and remove the carbon dioxide; this would be like flipping a light switch because we would be able to do 100 percent of the gas exchange for the patient. That’s something we haven’t seen done before.
MassDevice:How do you go about determining whether to create a device for the pediatric market, which is typically much smaller than for similar, adult-sized devices?
KD: The pediatric challenge is really an amazing challenge, because there are really not great economic reasons to pursue a pediatric device. The market is small and the liabilities are high. Nevertheless, we do have the ability to scale our technology down to be an ideal platform for pediatric patients. so we have centrifugal pumps are typically what we make. A centrifugal pump is probably the best of the various types of pumps to scale down for this size. Our first pediatric device is a polycarbonate plastic device based on the same bearingless motor mag-lev technology. We’ve taken a pump that was originally for adults and would have a 31ml fraction volume and scale it down to 14ml, half the size. That is our first entry into the pediatric market. We’ve done about 8,000 adult patients so far with the adult version and we’ve done about 600 pediatric patients so far with the PediVAS device.
The market is quite small. We’re estimating that with an implantable version for ventricular assist device for a pediatric population, there may be 100 per year with probably four or five companies developing technology for that particular field. For the acute market, that number is closer to 1,000 patients a year and maybe larger. A company could not go into this on its own. Fortunately, the National Institutes of Health have a very significant focus on pediatrics and also the Food & Drug Administration has the orphan product humanitarian use designation. We’ve pursued NIH funding and have been successful in getting significant funding from the NIH for PediVAS. We’ve also received the HUD designation from the FDA. So the bar has been lowered from a regulatory perspective and with the assistance of the NIH, which has made it possible to pursue this.
Our point of view is that we know we can develop the technology successfully, that these pediatric patients will benefit immensely from this development and the goodwill of supporting pediatric patients will also spill into the adult market. We’ve also developed a next generation beyond PediVAS, which is a titanium version where we’ve now scaled the pump size down from the original 31ml and then 14ml, now we’re down to 7.5ml from a pump that will do actually neo-nates to adults. This pump will do six liters a minute, so it’s highly versatile.
MassDevice: You’re also developing an external cardiac assist system. Where are you with that project? What’s the timeline for trials, regulatory applications, commercialization, etc.?
KD: We have full approval in Europe for CentriMag for left, right and bi-ventricular support, as well as for a technology called extracorporeal membrane oxygenation, ECMO, where you combine the ventricular assist device with an oxygenator and you can do both heart and lung. We are fully approved for up to 30 days. We have CE Mark for CentriMag, CE Mark for PediVAS for all these applications, and on the titanium version of the long-term device, we’re hoping to have a CE Mark next year, 2011. In the United States CentriMag has a 6-hour approval under a 510(k), but it also has a 30-day approval as a ventricular assist device to support the right side, under an HDE. We are in clinical trials to finalize a PMA, we have 18 patients left in our trial out of a total of 30. That’s an unusually small number, but we worked closely with the FDA and they understood that the market is a small market. Once we have the approval we would expand on these indications and move into other areas. With the pediatric device, an IDE has been submitted and we’re pending approval to do a 20-patient trial in the United States en route to an HDE, which then would be followed by a PMA.
MassDevice: Has the emphasis on due diligence as far as reimbursement goes changed over the years?
KD: It’s changed. Many years ago, we just assumed that if you had a great device and you were saving lives, that at the end of the day someone would buy it and that these things would take care of themselves. When we first created HeartMate many years ago, we really did very little in terms of preparing for reimbursement. Fortunately it was the first of its kind and there was a lot of interest in it. It got a lot of attention and it did get reimbursed, but the next-generation device was much more expensive and we realized very quickly on the second-generation device that we had to be very pro-active on reimbursement. Especially when you move from bridging patients to transplantation to destination therapy, and even more so now as these devices become more reliable and smaller and more cost-effective, as you try to back up in the disease scheme to less-sick patients where you’re going to see many more, then it becomes really critical to have a convincing argument as to why it’s safe, effective and can be afforded by society.
It’s absolutely critical. It’s something that companies often make a mistake in failing to address early on. It’s important, probably even before you begin a clinical trial, to begin thinking about your options. We work closely with [MassDevice blogger and reimbursement expert] Ed Berger on understanding what the current reimbursement environment is, prior to going into clinical trial, then trying to collect data and along the way make sure that at the end of the trial we’ve addressed what concerns the right people might have about how to go about reimbursing. We do rely heavily on Ed, he’s been wonderful. At Cardiosystems we retained Ed’s services many, many years ago and he really was instrumental in creating the whole reimbursement scheme for ventricular assist devices. He, along with another fellow by the name of Karl Nelson, out in Salt Lake City.
MassDevice: What’s your take on the impact of the 2.3 percent excise tax on medical devices contained the healthcare reform act?
KD: There’s going to be a lot of pressure to reduce pricing. I’ve seen estimates of a 30 percent reduction in pricing going forward. I expect that the manufacturers will have to eat [the excise tax]. Others may think that you’ll be able to just pass that along, but I doubt that will be the case. I think that is just part of the puzzle. In general we’re going to see great pressure to reduce prices and we’ll have to deal with all of these issues in our strategies going forward. I’d expect that our prices are going to have to erode.
I’m certainly not the expert in this area, but that’s the impression I’ve been getting in speaking with my colleagues. It could force consolidation in a field like ours. I think you’re going to see companies starting to merge to deal with this situation and get more efficient. The taxes are a small part of it. I have frequent opportunity to speak to some of the analysts down on Wall Street who are really watching companies going forward and this is going to affect not only the medical device industry, but the venture capital industry. It’s going to affect a large group of individuals and companies. Hospitals have really cut back as much as they can in many respects, on labor, and so there’s been a major emphasis on pharmaceuticals and budget cuts there and that will stay. But the attempts to really reduce the cost of medical devices is really only just beginning. So if you don’t have labor [costs] and you’re watching your supplies, then the only big-ticket items are pharmaceuticals and medical devices. There’s going to be a lot of pressure to look at the most cost-effective places. There’s some discussion of comparing efficacy of devices. If you’ve got a device that’s $5,000 and another that’s $200 and they’re roughly equivalent in terms of effectiveness, what’s going to happen? I think there’s going to be a lot more pressure to focus on cost-effectiveness. And therefore its going to create competition and you’re going to have to compete by having a great device and you’re still going to have to compete on your pricing.
I’m a glass-half-full kind of guy, but it doesn’t sound like it, does it? What’s the difference between an optimist and a pessimist? A pessimist has more experience. So that doesn’t sound very half-full. But I am far from an expert in this area.

