An FDA panel yesterday recommended that the FDA reclassify membrane lung for long-term pulmonary support systems, or so-called extracorporeal membrane oxygenator circuits and accessories, from the highest-risk Class III category to the less burdensome Class II, with special controls.
ECMO systems, which have been available for around 30 years, provide assisted extracorporeal circulation and physiologic gas exchange of a patient’s blood when an acute reversible respiratory or cardiac condition prevents the patient’s own body from providing the physiologic gas exchange needed to sustain life, according to the FDA.
Doctors use ECMO systems as a last resort for patients who are unresponsive to optimal ventilation or pharmacologic management. As pre-amendments Class III devices, they currently require a 510(k) to get to market rather than the more burdensome pre-market approval required of Class III devices.
In effect, ECMO systems already are Class II devices, because they are currently regulated as such, the panel pointed out.
"I want to address 2 comments. One is, how poorly individuals do who receive ECMO therapy," said Dr. Richard Lange of the University of Texas in San Antonio. "These are devices that are usually put in as a very last choice of treatment for individuals who fail medical therapy, and there really is no other therapy thought to be available to sustain their life, either for a reversible condition that they can get over, or a definitive therapy. So, it’s sobering that patients do not do very well, but absent this, the thought is, as my colleagues mentioned, they would die.
"The other issue was the issue of the changing device," Lange said. "That’s actually, from a medical standpoint, a positive. These devices continue to improve. They continue to improve with their manufacturing process, their safety. The industry takes whatever their current use is and troubleshoots to find out what problems are occurring, so it’s safer for the patient and it’s more effective as well, and this is a therapy that has matured. So, even though the oxygenators are different than they were 4 or 5 or 6 years ago, they’ve matured and the devices are actually presumably better. Industry doesn’t take 2 steps back to make a worse device."
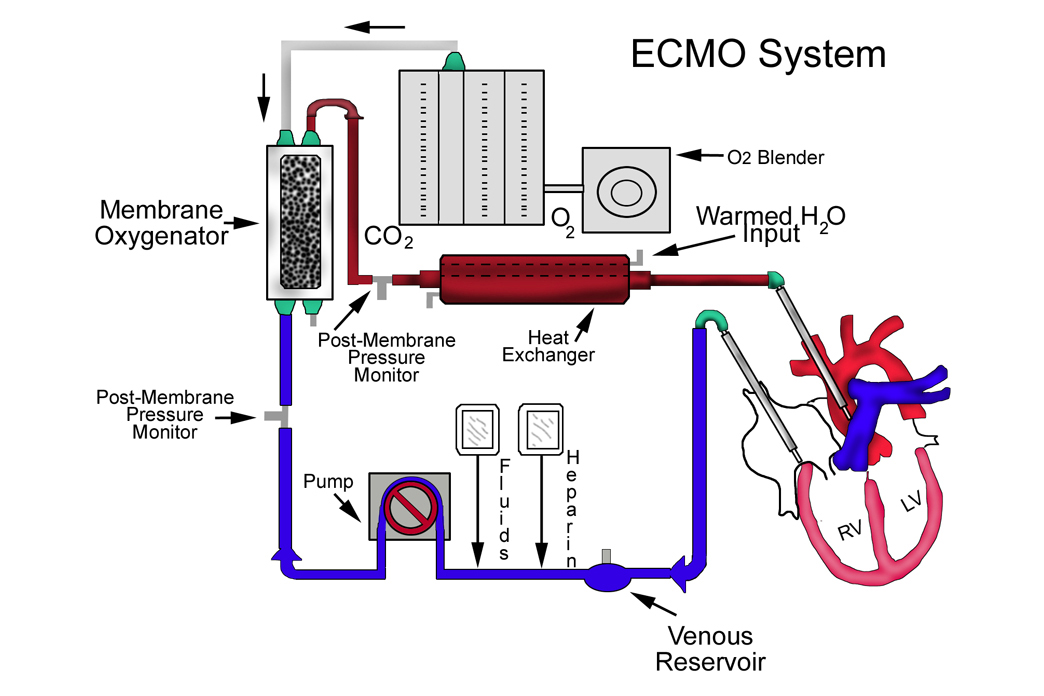
ECMO systems include an oxygenator, blood pump, cannulae, heat exchanger, tubing, filters, monitors/detectors, and other accessories; and the circuit components and configuration may differ based on the needs of the individual patient or the condition being treated, the FDA said.
Despite a long list of risks to health associated with ECMO therapy, including thrombocytopenia, hemolysis, adverse tissue reaction, inadequate gas exchange, gas embolism, mechanical failure, hemorrhage, hemodilution, thrombosis/thromboembolism, infection and mechanical injury to access vessels, a majority of panelists said the benefits of ECMO outweigh its risks.
ECMO therapy is safe and effective, according to the FDA’s definition of those terms, the panelists agreed, although they expressed discomfort with calling a therapy with so many associated health risks "safe." Rather, the risk-benefit ratio is right, panelists said, because absent the use of ECMO therapy, the option is death.
Data presented to the panel was primarily from neonates and infants. Though ECMO therapy is also used for adults, robust evidence on use of the therapy in adults is lacking, and panelists said they could not come to a conclusion on use of ECMO for adults for this reason.
If the FDA follows the panel’s recommendation to reclassify ECMO to Class II subject to 510(k) clearance and special controls, as the agency itself proposed to do Jan. 8, the therapy could continue to be used in adults.
"We have been presented data with regard to pediatrics for the indications that were brought forward," said panel chairman Dr. Richard Page of the University of Wisconsin School of Medicine and Public Health in Madison. "There has been concern raised by the panel that we have not had the opportunity to review adult data, and we have given good guidance to the FDA in terms of the need to fully vet the data for adults."
Panelists advised the FDA that is "imperative" that the panel and the agency adequately examine clinical data on use of ECMO in adults in a future advisory panel.
What it means for industry
In an interview with MassDevice.com after the panel, ALung senior vice president for regulatory affairs Frank Falcione said the panel’s recommendation has not added clarity for his company and could create problems for other manufacturers of component devices used in ECMO therapy.
ALung makes the Hemolung, an extracorporeal carbon dioxide removal system that works by removing carbon dioxide and delivering oxygen directly to a patient’s blood via a small catheter inserted into the jugular or femoral vein. It’s already on the market in Germany, France and the U.K. ALung recently raised $15.8 million to accelerate its commercialization.
"They’ve basically said, ‘You, gas exchange company, can now go and put in a 510(k), but it doesn’t really address which pump you use, which heat exchanger you use, which oxygenator you use,’" Falcione said. "So if I was a manufacturer of just an oxygenator, I would have a little bit of difficulty because of compatibility issues, because there are 45 heat exchangers out there, there are 150 different pumps.
"So if I go to the FDA now under this new regulation, are they going to come back and say what other manufacturers’ devices work with your device from a compatibility standpoint?" he said. "Most of us would not be able to go out and buy those, because we’re not a customer, so even though it’s going to be a 510(k), it’s probably going to be put on some sort of testing regimen that you may or may not be able to do."
Furthermore, the panel’s recommendation, which focused on pediatric indications for ECMO, failed to provide insight into an approval strategy for ALung specifically, he noted.
"The primary reason that we came here, what all the confusion was about, is the adult indication," Falcione said. "We’re in the process of submitting an [investigational device exemption] right now. The amount of time for the approval of the IDE and how long it’s going to take us to conduct the study, is that going to be in the same time frame of the FDA changing this from a PMA submission to a 510(k)? I don’t think that’s clear."

