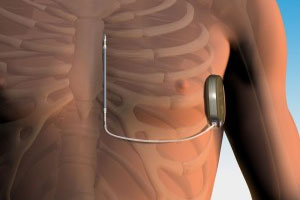
Cameron Health’s under-the-skin defibrillator may take longer to respond to cardiac events than standard implantable cardiac defibrillators, but speed isn’t always the most important factor in saving a life.
Although Cameron’s S-ICD took longer than 18 seconds to respond in 12% of patients in the ongoing Effortless study, it always responded in time with life-saving therapy and did so while delivering fewer inappropriate shocks to the heart.
"If this study were presented 5 years ago, everyone would say, ‘We’d never program our devices that way; this is going to kill people,’" Dr. Derek Exner, who attended one of Cameron’s S-ICD sessions at the Cardiostim conference in France, told TheHeart.org. "Now we’re seeing that we’re treating a lot of patients who don’t need to be treated and getting these huge rates of inappropriate therapy, and now the mindset has switched and says that longer is better."
The Effortless study, which includes 219 patients so far, had 50% fewer instances of inappropriate shocks than the clinical trials that won the S-ICD a near-unanimous recommendation from the FDA’s circulatory devices panel.
Earlier studies showing higher rates of unnecessary shocks may have been related to physicians skipping important steps in programming the device and selecting appropriate patients, according to a pair of physicians who presented data at the Cardiostim conference in this week.
Dr. Gust Brady, credited with inventing Cameron’s S-ICD, told attendees that physicians in early clinical trials implanted the device in patients whose heart rhythms were outside the preferred pattern recommendations, which a physician can check with a heart rhythm range test provided with the S-ICD system, according to the website.
"If you cheat and try to sneak a patient in that doesn’t pass this test, you’ll have false-positive shocks," Bardy said.
Physicians in earlier clinical trials may also have failed to program the device’s shock zones, which define what types of rhythms the device should consider dangerous enough to merit a shock, according to Dr. Michael Gold, who participated in the device’s early trials.
With proper programming, rates of inappropriate shocking will become "vanishingly low," Gold said.
The device reacted with a shock and reversed abnormal heart rhythms 100% of the time in the study, with a 7% rate of unnecessary shocks. Rates of device-related complications were 2.2% and procedure-related complications were 12.2%.
Boston Scientific (NYSE:BSX) sealed the deal earlier this month with Cameron in a merger worth up to $1.35 billion.

