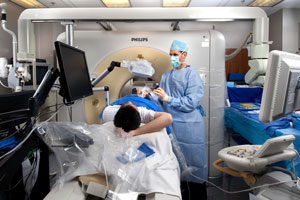
Congress agreed to cut Medicare reimbursement for certain medical imaging services, a move that could harm patients and drive up healthcare costs, according to imaging technology advocates.
The fiscal cliff package included another in a series of reimbursement slashes for imaging services in recent years, despite a decrease in imaging use by Medicare beneficiaries, according to the Access to Medical Imaging Coalition.
"Congress is blindly slashing Medicare payments for diagnostics without true knowledge about how their previous cuts affect seniors’ access to early diagnosis services," AMIC executive director Tim Trysla said in prepared remarks. "By putting in place yet another payment cut for imaging, Congress has further reduced patient access to vital early diagnosis that we know saves lives."
Legislators have approved 8 cuts to medical imaging reimbursement in the last 6 years, according to the Medical Imaging & Technology Alliance.
As a result, per-beneficiary Medicare spending for imaging has already decreased 13.2% since 2006 and payments for some services, such as brain MRIs, have been cut by more than 60%, MITA reported.
"We know that cuts which already have gone into effect have forced physician practices and providers to scale back on clinical staff and forgo technology upgrades," Trysla added. "This additional cut will further exacerbate those problems closing additional free-standing imaging centers and forcing patients to either forgo life-saving imaging or receive a scan in hospitals where they are more expensive."

